Tutorials:
- Birth of
the baby
- Birth of
the placenta
- Local anesthesia for vaginal/
perineal repair
- Repair of the Perineum
|
Tutorial 2: Birth of the Placenta
Birth of the Normal Placenta During Childbirth
2. Normal Anatomy and Physiology of the Third Stage of Labor
- Process of placental growth and uterine wall changes during pregnancy
- The placenta grows with the placental site during pregnancy.
- During pregnancy and early labor the area of the placental site probably changes little, even during uterine contractions.
- The semirigid, noncontractile placenta cannot alter its surface area.
- Anatomy of the uterine/placental compartment at the time of birth
|
- The cotyledons of the maternal surface of the placenta extend into the decidua basalis, which forms a natural cleavage plane between the placenta and the uterine wall.
|
|
|
- There are interlacing uterine muscle bundles, consisting of tiny myofibrils, around the branches of the uterine arteries that run through the wall of the uterus to the placental area.
|
|
- The placental site is usually located on either the anterior or the posterior uterine wall.
|
|
- The amniotic membranes are adhered to the inner wall of the uterus except where the placenta is located.
|
- The process of placental separation during and after birth
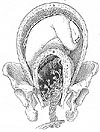 |
- The surface area of the uterine cavity gradually increases during pregnancy and rapidly decreases during the second stage of labor.
|
|
- Separation involves a slow, progressive detachment from the uterine wall brought about by the physical changes which occur during and after the actual birth of the baby.
|
|
- The placenta is separated from the decidual attachment by the action of the uterine muscle.
- As the baby gradually leaves the uterus, the cavity of the uterus must become progressively smaller to permit the uterine wall to remain closely approximated to the baby. This maintains the expulsive force of the muscular contractions on the body of the baby.
- The mechanism for achieving this close approximation is through a slight shortening or retraction of the individual muscle fibers during each contraction. Slow delivery of the shoulders and body of the infant will permit the muscle fibers to retract and adjust to the reduction in size of the cavity, thereby promoting more efficient contractions.
- As the surface area of the interior of the uterus slightly reduces the diameters of the placental site, the placenta becomes thicker and decreases slightly in diameter.
- Since the placenta has a limited ability to alter its surface area, it must separate if the area to which it is attached is reduced considerably in size.
- The separation, which occurs in the outer portion of the spongy layer of the decidua basalis, begins during the later second stage of labor and is usually completed as the uterus contracts during the final expulsion of the baby.
|
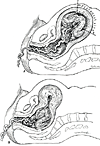 |
- The effectiveness of this process depends on the extent to which the placental site is reduced. If the contractions are firm and forceful, the placenta may be expelled almost immediately after the baby is born. However, if they are less effective, complete placental separation may be delayed.
|
|
- The blood sinuses at the placental site, which have been opened by partial or complete separation of the placenta, are the source of bleeding during and after the third stage of normal labor. This bleeding is controlled initially by firm contraction of the interlacing uterine muscle bundles around the branches of the uterine arteries.
- the vessels are compressed and kinked
- bleeding from the open ends is slight
- if the uterine muscle is relaxed, the bleeding will be brisk and continuous.
|
- The process of expulsion of the placenta after separation - Expulsion of the placenta is a function of abdominal, uterine, and gravitational forces and cord traction by the attendant.
|
- After separation, blood accumulates behind the placenta, and the uterus rises in the abdomen. A firm uterine contraction now begins, and the uterus changes from a flattened, soft, discoid organ to one that is firm and globular. This process can take from several minutes to much longer, depending on the strength of the uterine contractions and the location of the placenta within the uterus. A lower implantation will mean less firm contractions in the lower uterine segment and a longer time for separation and expulsion.
|
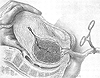 |
- During a uterine contraction, the flattened uterine body of the uterus becomes globular as the placenta is forced downward into the lower uterine segment.
- As the placenta leaves the upper part of the uterus, the uterus can be felt through the abdominal wall as a hard, globular mass.
|
 |
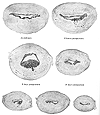
- Birth of the placenta by the Schultz Mechanism
- The fetal surface of the placenta slips through the opening in the fetal membranes and appears at the introitus.
- The membranes then peel off the surface of the uterine cavity, uniformly and intact.
- The liquid blood and retroplacental clots, if any, are contained within the folded placenta and are not evident until the placenta is delivered and examined.
- Birth of the placenta by the Duncan Mechanism
- One edge of the placenta first slips through the cervix and into the vagina. The remainder of the placenta follows, and the fetal membranes are peeled from the uterus as traction is made on the edge of the placenta which follows.
- The liquid blood and retropalcental clots escape from the uterus as the maternal surface of the palcenta is delivered.
- The Duncan Mechanism is more frequently followed by retained fragments of the fetal membranes.
|
|
- Uterine contractions continue, with the muscle fibers creating living ligatures to provide hemostasis.
|
- Immediately following the birth of the placenta
- The contracted body of the uterus forms a hard globular mass, the apex of which is about midway between the umbilicus and symphysis.
- This solid mass of tissue contains a flattend cavity with anterior and posterior walls in close apposition, each measuring 4-5 cm in thickness.
- Because of its compression by the contracted myometrium, the uterus appears anemic, as contrasted with the purplish pregnant uterus.
- A portion of the decidua, which remains, has an irregular jagged appearance, and marked infiltratioln with blood, especially at the placental site.
- Extrusion of the placental site takes up to six weeks.
 |
- After delivery, the placental site is an irregular, nodular, elevated area about the size of the palm of the hand.
- By the end of the second week the placental site measures 3 to 4 cms in diameter.
- Williams describes the process as follows:
|
Involution...."is not effected by absorption in situ, but rather by a process of exfoliation which is in great part brought about by the undermining of the placental site by the growth of endometrial tissue.... Such a process of exfoliation should be regarded as very conservative, and as a wise provision on the part of nature: otherwise great difficulty might be experienced in getting rid of the obliterated arteries and organized thrombi which, if they remained in situ, would soon convert a considerable part of the mucosa into a mass of scar tissue with the result that after a few pregnancies it would no longer be possible for it to go through its usual cycle of changes, and the reproductive career would come to an untimely end."
Williams, J. W. Regeneration of the uterine mucosa after delivery with especial reference to the placental site. Amer J Obstet Gynec 22:664, 1931. |
click on the links below to continue:
- Introduction
- Normal Physiology of the third stage
- Anatomy and Variations of the normal placenta
- Procedures for the birth of the normal placenta
- End Note
|